Using Conservative Interdisciplinary Case Management to Enhance Success Through Future Risk Reduction
Raj Upadya, DMD; Eric C. Weiss, DMD; Jason T. Rothenberg, DMD
Interdisciplinary treatment poses unique challenges for even the most astute clinicians; however, its implementation is critical for ensuring a successful functional, biologic, and esthetic outcome. The restorative dentist must act as the "quarterback" to coordinate complex treatment strategies with the team of specialists. In contrast, a multidisciplinary approach typically involves individual specialists working in isolation to achieve a specific objective without necessarily envisioning the overall end result. While some aspects of the therapy may be successful, the overall treatment may be more likely to fail and disappoint the patient. This article demonstrates how a conservative interdisciplinary plan can be successfully developed and implemented.
Planning for Success
The first step is the performance of a full examination; it is complete when the clinician has identified all potential causes of poor oral health or function (Table 1). The seven goals of complete dentistry,1 as described by Dawson, are: 1) freedom from disease in all masticatory structures; 2) maintainable healthy periodontium; 3) stable temporomandibular joints (TMJs); 4) stable occlusion; 5) maintainable healthy teeth; 6) comfortable function; 7) optimum esthetics.
Unstable TMJs result in an unstable occlusion. Their diagnosis will help determine if the restorative position should be centric relation (CR), adapted centric posture (ACP), or maximum intercuspation (MI). CR by definition is the stable, reproducible location where the lateral pterygoids release, elevator muscles contract, and the healthy condyle-disk assemblies are in their most superior/midmost position of the glenoid fossa, against the eminentiae, their medial poles braced by bone.2,3
The complete examination is supplemented with vital diagnostics including full-mouth and panorex radiographs, CT/MRI (if appropriate), photographs, study models, and facebow and CR bite records. The clinician should search for stability and instability during the examination (Table 2). The TMJs are considered stable for occlusal therapy if any noted disorders are extracapsular or involve only lateral pole disk displacement (Piper TMJ Class IIIB or lower). If medial pole derangement of the articular disk is diagnosed (Piper Class IVA or higher), then long-term splint therapy is considered appropriate before changing the occlusion. With a complete examination, most temporomandibular disorders can be stabilized; failure to address this issue prior to treatment may have devastating effects on newly placed porcelain restorations.4-6
Changing the Lineup
Standard treatment strategies typically address biologic issues first (eg, stress from microorganisms), then focus on structure and function, and finish with optimization of esthetics. Considering esthetics last increases the likelihood of a disappointing result for the patient. For this reason, the authors recommend the facially driven approach: Begin with the end in mind. Start with esthetics and work backward to biology. Nothing will be excluded; strategic planning will simply be reversed.7 Crucial to this type of approach is the use of diagnostic photographs, similar to how radiographs are used for evaluating structure.
The amount of normal resting maxillary incisal edge display decreases with age due to gravity's effect on the soft tissues.8 With the guidance of photographs, the vertical incisal edge position of the maxillary centrals is planned relative to the upper lip, using standard "E" and rest position views. The trajectory of the incisors and horizontal placement of their incisal edges are equally important, determined relative to the inner vermillion border of the lower lip and the lip closure path using profile smile and tilt-down smile views (Figure 1 and Figure 2). Errors in incisal edge placement can result in problems with phonetics, the neutral zone, and envelope of function. This may also lead to xerostomia and overall patient discomfort.9-11
The 4x4 Approach
The esthetic plan is subsequently integrated with function after evaluation of the TMJs and mastication muscles. The records from the examination are transferred to a semi-adjustable articulator for mounted model analysis. Using a combination of adjustment of the models and wax-ups, the esthetic plan is transferred to the casts.3,7This type of visualization facilitates thinking "outside of the box," which may help identify minor orthodontic and/or periodontic interventions to improve overall esthetics. This type of conservative treatment can also lower overall risk significantly.
Effective interoffice collaboration will help ensure positive clinical and nonclinical experiences for patients throughout treatment.12 The wax-up is perfected for function and esthetics by the laboratory and helps to guide provisionalization. This conveys important information to assist specialists in envisioning common goals and enhancing clinical outcomes. Provisionals are "road tested" in the patient, confirming predictions, and used more like prototypes than temporaries. It is far easier and less disheartening to make adjustments in acrylic or bis-acryl, compared to fresh porcelain. After esthetics, function, comfort, and speech have been confirmed, photographs, casts, and facebow of the approved prototypes are sent to the laboratory for duplication in the definitive materials. The result is minimal chairtime for delivery and virtually no adjustments, because, in actuality, the case has been done four times: in the mind, in wax, in provisionals, and in the definitive materials.
Clinical Case
A 50-year-old male complained of loose upper four-unit bridges placed 15 years ago and sensitivity of anterior teeth. An examination revealed recurrent caries of the terminal abutments of both restorations (Figure 3). Dental history included extraction of both distal terminal abutments of the previous three-unit bridges due to caries and failed endodontics. They were replaced with the currently failing fixed partial dentures. Teeth Nos. 20 and 31 had been previously extracted due to fracture. The medical history included maxillary sinus antrostomies to relieve chronic sinusitis approximately 20 years earlier. Social history included several cigars daily.
The patient was concerned that new bridges could similarly fail and was averse to removable prosthetics. He wanted to reduce risk, increase function, and improve his esthetics while having individual teeth. Initial analysis revealed several signs of instability (Table 2): CR-MI discrepancy and posterior working and balancing interferences during protrusive and lateral movements of the mandible were recognized. These were thought to be largely responsible for the noted damage (Figure 4, 5, 6, 7, 8). Records were prescribed to accurately diagnose the condition and develop a treatment blueprint.
Muscle palpation findings revealed medial and lateral pterygoid tenderness and hypertrophic masseters. TMJs were able to accept firm bilateral load testing using bimanual manipulation. Doppler ultrasound and joint vibration analysis confirmed bilateral Piper Class II joints, with intermittent reciprocal staccato clicks and mild crepitus. CR-MI discrepancy was verified with mounted models (Figure 9).
Goals, Treatment Plan, and Discussion
The goals included achieving CR-MI with even tooth contact, canine guidance to disclude all posterior teeth with smooth transition to the anterior guidance, and protrusive guidance with no posterior interferences. The objectives also involved maximizing functional esthetics to mimic nature while reducing overall risk and fulfilling the patient's wish for individual restorations.
To correct damage and minimize risk of fracture of unsupported porcelain, full-coverage restorations with substructures were planned for teeth Nos. 7 to 10 and 19 to 30. Pontics for teeth Nos. 4, 5, 12 and 13 would be replaced with implant restorations, and single crowns were planned for teeth Nos. 3, 6, 11 and 14. Analysis of the maxillary anterior teeth revealed unesthetic gingival levels. It also showed that preparation for full-coverage restorations designed to maximize functional esthetics would result in iatrogenic pulpal exposure or a future need for endodontics. This assessment determined the need to involve orthodontic and periodontal specialists, and the first of several team "huddles" began.
The patient consulted the periodontist for eventual implant placement in the maxillary premolar positions. A comprehensive periodontal evaluation had revealed no significant disease activity. Probing depths were 3 mm or less, with few signs of inflammation.
Next the patient was referred for a cone-beam tomography scan of the maxilla to evaluate the alveolar dimensions and the maxillary antra, which were thought to be inadequate (Figure 10 and Figure 11). Because radiographic studies showed maxillary sinus thickening, the patient was referred to his otolaryngologist, whose diagnosis was: "rule out ethmoid sinusitis, bilateral maxillary sinusitis with sinus cyst." Subsequent procedures were: "ethmoidectomy, bilateral revision, endoscopic, maxillary sinusotomy, endoscopic revision and ENTrak," after which the patient was cleared to proceed with sinus elevation surgery.
Cone-beam evaluation revealed approximately 5 mm of alveolar bone on the right. Because the right side demonstrated inadequate bone dimensions for simultaneous placement of implants, a lateral window sinus graft was completed first. Removing the existing bridge beforehand was not necessary because access was not impeded.13,14The lateral window-type sinus elevation was therefore performed using a combination of xenograft and allograft (Figure 12).
After sinus grafting was completed, the patient consulted the orthodontist for finalization of an orthodontic plan in anticipation of anterior restorations and implants in the premolar positions. The patient's structure was a skeletal Class II with mild maxillary crowding. The upper central incisors were retroclined while the lateral incisors were proclined. The mandibular arch was well aligned, although the lower midline was shifted to the patient's left with the cuspids in a Class II relationship. The plan was to align the upper incisors and level the incisor gingival margins before the placement of restorations.
The ideal orthodontic treatment plan would include maxillary and mandibular fixed appliances to accomplish the aforementioned goals, as well as to idealize the spacing required to replace teeth Nos. 20 and 31, with uprighting of the lower molars. This would also allow correction of the left cuspid relationship to a Class I and the development of anterior guidance. The patient refused not only fixed appliances but also any treatment involving the mandibular arch. Clear aligners would be used to align the maxillary incisors and level the gingival margins.
Impressions were submitted for computerized design and fabrication of the aligners. Nine aligners were necessary. To assist in resolution of the crowding without flaring the incisors, interproximal reduction of 0.2 mm between teeth Nos. 7 and 8, Nos. 8 and 9, and Nos. 9 and 10 was prescribed. The patient was instructed to wear each aligner 20 hours daily for 2 weeks. This series was completed in 18 weeks. A small discrepancy remained in the alignment of the incisors; the patient was offered a refinement, but refused further orthodontics.
After completion of the desired tooth movement (Figure 13 and Figure 14), new diagnostic records were obtained. Then, provisionalization and occlusal equilibration were performed. To ensure occlusal stability, function and esthetics were refined during three visits, spanning 8 weeks.
At this point, 6 months of healing had passed since the sinus graft, and the site was cleared for implants. The left side had more initial bone, thus it was determined that simultaneous internal sinus elevation could be performed.15 Recommendations by Fugazatto for length of implants placed at the time of an internal osteome-type sinus elevation were followed.16 The implants (4.1 mm diameter with a Regular Neck size platform, Straumann, https://www.straumann.us) were placed in the maxillary premolar positions, with an internal sinus elevation completed on the left side (Figure 15 and Figure 16). Clinical crown lengthening was also performed to ensure adequate ferrule for tooth No. 6, resulting in a slight variance from ideal gingival esthetics. One unique design component of the implants used in this case is a transgingival collar, which allows a "one-stage" type placement, removing the need for a second surgical procedure to expose the implants. It also eliminates the potential for a microgap, as the abutment/implant interface is significantly superior to the crestal bone.
After two months of healing, the maxillary provisionals were sectioned distal to the cuspids, and the solid abutments were used to help develop the soft-tissue emergence (Figure 17). In the interim, final zirconia restorations for teeth Nos. 22 to 27 and Nos. 6 to 11 were placed. Some compromises were made because the patient declined conventional orthodontics and any periodontal procedures suggested for purely esthetic reasons. Thus, a bridge to replace tooth No. 20 was prescribed, and tooth No. 31 was not replaced. The porcelain-fused-to-metal (PFM) high-noble (HN) bridge for teeth Nos. 19 to 21 and PFM-HN crowns for teeth Nos. 28 to 30 were inserted next. This was followed by placement of PFM-HN crowns for teeth Nos. 3 and 14 and implant PFM-HN crowns for teeth Nos. 4, 5, 12, and 13.
Proper diagnosis and conservative interdisciplinary planning occurred before any treatment commenced. Therefore, the reconstruction was successfully completed in several succinct visits, with no adjustments made during insertion of the final restorations (Figure 18, 19, 20, 21, 22, 23).
Conclusion
This complex interdisciplinary case was thoroughly, efficiently, and thoughtfully completed as a result of good treatment planning and communication. Low-exposure cone-beam tomography is relatively inexpensive and provides significant diagnostic capabilities. Sophisticated software allows for simulated surgery and implant placement, as dictated by the restorative treatment plan. The evolution of sinus augmentation surgery now enables implants to be successfully placed and restored in anatomic areas that were previously deemed untreatable. Surface technologies of implants have increased the amount of bone-to-implant contact and decreased the time needed for osseointegration. Implants with transmucosal collars facilitate the elimination of second-stage surgery to uncover submerged implants.
Clear aligner therapy has become mainstream for accomplishing minor tooth movement in lieu of fixed appliances. When it is not imperative to idealize the alignment and occlusion orthodontically, clear aligners can be used to provide basic alignment, thus alleviating the needs of the restorative dentist. These techniques allow more ideal contours of restorations and enable more conservative preparations.
Treatment planning for a complicated case has multiple potential approaches. If complete diagnostics are attained and case planning envisions the end result, esthetics can be greatly improved. Carefully orchestrated, conservative specialist involvement may also reduce risk and enhance clinical outcomes, ultimately increasing patient satisfaction.
References
1. The concept of complete dentistry. In: Dawson PE, ed. Functional Occlusion: From TMJ to Smile Design. 1st ed. St. Louis, MO: Mosby; 2007:4-9.
2. Dawson P. Centric Relation. In: Dawson P, ed. Functional Occlusion: From TMJ to Smile Design. 1st ed. St. Louis, MO: Mosby; 2007:57-68.
3. Spear F. Occlusion in the new millennium: the controversy continues. Spear Signature. 2002;7:18-21.
4. Cranham J, Dawson P. Relating occlusal treatment to Dawson classification. Vistas: Complete and Predictable Dentistry. 2010;3(1):12-18.
5. Hess L. Pre-restorative diagnosis. Inside Dentistry. 2010;6(6):44-54.
6. Hess L. Restoring the functional zone: correcting anterior constriction with centric relation-based. Inside Dentistry. 2007;3(9):74-79.
7. Spear F. Interdisciplinary management of anterior dental esthetics. Advanced Esthetics & Interdisciplinary Dentistry. 2006;2(4):6-19.
8. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
9. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, IL: Quintessence; 1994:21.
10. Dawson P. Evaluation, Diagnosis and Treatment of Occlusal Problems. 2nd ed. St. Louis, MO: Mosby; 1988:330.
11. Cranham J. The horizontal position of the maxillary incisal edge: the key to optimum esthetics, phonetics and function. Contemporary Esthetics and Restorative Practice. 2006;10(2):22-24.
12. Levin R. Secrets to effective GP/specialist relationships. Inside Dentistry. 2010; 6(6):32-34.
13. Tatum OH Jr, Lebowitz MS, Tatum CA, et al. Sinus augmentation. Rationale, development, long-term results. N Y State Dent J. 1993;59(5):43-48.
14. Wallace SS. Lateral window sinus augmentation using bone replacement grafts: a biologically sound surgical technique. Alpha Omegan. 2005:98(2):36-46.
15. Summers RB. A new concept in maxillary implant surgery: the osteotome technique. Compend Contin Educ Dent. 1994;15(2):152-156.
16. Fugazzotto PA. Treatment options for augmentation of the posterior maxilla. Implant Dent. 2000;9(3):281-287.
 Figure 1 Profile smile. |  Figure 2 Tilt-down smile.  Figure 3 Full-mouth radiographs. Note location of maxillary sinuses, as well as mesial angulation of teeth Nos. 19 and 32. | |||||
 Figure 4 |  Figure 5 | |||||
 Figure 6 |  Figure 7 | |||||
 Figure 8 | ||||||
| Figure 4 through FIgure 8 Initial photographs. Note pathologic loss of enamel depicting occlusal disease. | ||||||
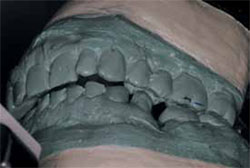 Figure 9 Diagnostic cast mounted on semi-adjustable articulator. Note significant CR-MI discrepancy. | ||||||
 Figure 10 Preoperative cone-beam scan, right side. |  Figure 11 Preoperative cone-beam scan, left side. | |||||
 Figure 12 Postsurgical panorex, depicting right side sinus graft. |  Figure 13 Postorthodontic results, anterior view. | |||||
 Figure 14 Postorthodontic results, maxillary occlusal view. |  Figure 15 Postoperative PA radiograph after implant integration showing right side, in site of lateral window sinus elevation. | |||||
 Figure 17 Provisionals after relining to incorporate solid implant abutments. |  Figure 16 Postoperative PA radiograph after implant integration showing left side, in site of internal sinus lift. | |||||
 Figure 18 Two-year follow-up of completed interdisciplinary reconstruction: panorex. |  Figure 19 Two-year follow-up of completed interdisciplinary reconstruction: full smile. Note harmony of incisal edges with lip line. | |||||
 Figure 20 Two-year follow-up of completed interdisciplinary reconstruction: tilt-down smile. |  Figure 21 Two-year follow-up of completed interdisciplinary reconstruction: profile smile. Note trajectory of incisors showing correct horizontal position of incisal edges. | |||||
 Figure 22 Two-year follow-up of completed interdisciplinary reconstruction: anterior, retracted. | ||||||
 Figure 23 |  Figure 24 | |||||
| Figure 23 and Figure 24 Two-year follow-up of completed interdisciplinary reconstruction: occlusal views. | ||||||
 |  | |||||
| ||||||




